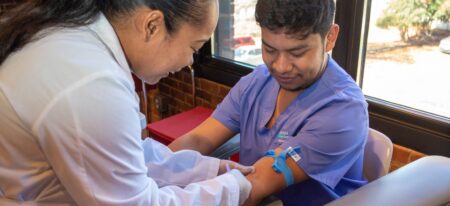
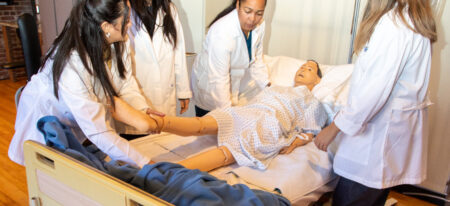
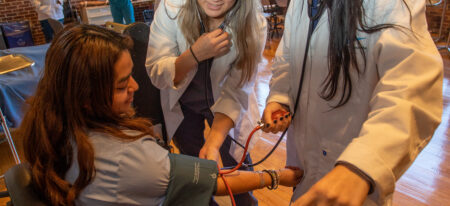
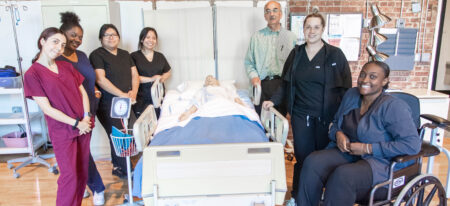
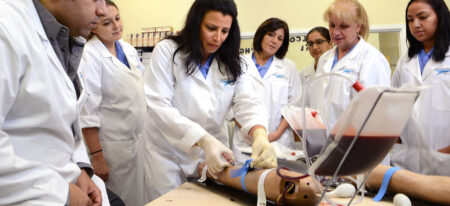
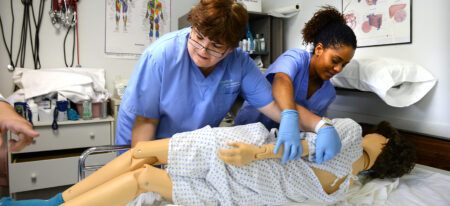
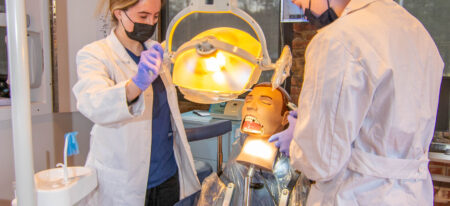
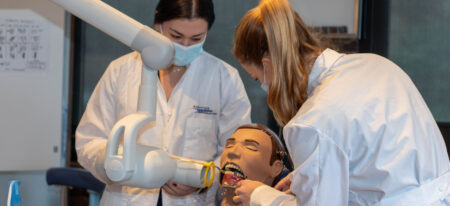
A New Beginning, We Change Lives
ACI Blog
Contact ACI Medical & Dental School
Contact us today for more information about finding the program that is right for you and enrolling at ACI Medical & Dental School.
Every accomplishment starts with the decision to try.
- Gail Devers
It only takes one person to change your life: YOU
- Ruth Casey
Ambition is the first step to success. The second is action.
- Unknown
I'm not telling you it's going to be easy, I'm telling you it's going to be worth it.
- Art Williams
You never fail until you stop trying.
- Albert Einstein
The only time you should ever look back is to see how far you've come.
- Unknown
The secret of getting ahead is getting started.
- Mark Twain
Believe you can and you're halfway there.
- Theodore Roosevelt
A dream written down with a date becomes a goal.
A goal broken down into steps becomes a plan.
A plan backed by action makes your dreams come true.
- Greg S. Reid
The secret of success is knowing where you are in life, asking good questions, then doing the next right thing.
- Frank A. Preston
If it doesn't challenge you, it won't change you.
- Unknown
Never stop learning because life never stops teaching.
- Unknown
Footer
ACI Medical & Dental School
GI Bill® is a registered trademark of the U.S. Department of Veterans Affairs (VA). More information about education benefits offered by VA is available at the official U.S. government Web site at https://www.benefits.va.gov/gibill.